UPDATED POST: This post was updated on Feb. 10, 2017 to include a link to the peer-reviewed national ferritin study publication, provide implementation dates and add clarification about ferritin testing feasibility.
The health and well-being of our donors is a top priority at Canadian Blood Services.
Health screening, education and donor testing help to ensure donors are healthy enough to give and that their gift doesn’t cause harm to themselves or to patients. If a problem is detected, we let donors know and advise to them to take action.
Checking hemoglobin is just one step to see if donors are healthy enough to give. Passing a finger prick hemoglobin test means a donor has sufficient levels of hemoglobin to donate blood. However, in early stages of iron deficiency, one can have normal hemoglobin, but low iron stores.
Your body uses iron to make hemoglobin, the protein molecule in your red blood cells that carries oxygen to your organs and tissues.
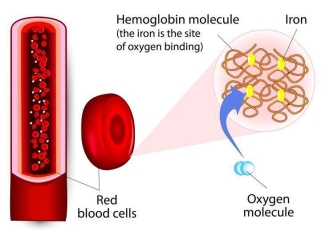
Iron deficiency is a common problem for many, in particular women of child-bearing age, where iron stores can be low, even prior to donation. A diet rich in iron is recommended for all blood donors, however, it can be difficult to meet and maintain the iron needs of blood donation, particularly for female donors, and donors donating several times a year.
How can we mitigate iron deficiency in blood donors?
Dr. Mindy Goldman, medical director of donor and clinical services, has been trying to find out the best ways to mitigate iron deficiency in blood donors.
Following an initial study of donors in Ottawa, she and her research team began a larger, more representative national ferritin study to further understand iron deficiency in Canadian donors and identify possible ways to address it.
The study comprised thousands of donors at a selection of clinics across the country. Donors were informed in the usual pre-donation pamphlet that their iron (ferritin) levels may be tested. To those who had ferritin levels in the low range, a letter was sent with an information sheet. Donors were advised to go to their doctor for further investigation and to get advice about iron supplements. They were also advised to have their ferritin level rechecked by their doctor before returning to donate.
Excerpt from the letter: “A low ferritin level means that you are not obtaining enough iron to meet your needs. Since blood donation leads to iron loss, it is possible that your low iron reserves are due to frequent blood donation. However, there are other causes of low ferritin, including a diet low in iron, trouble absorbing iron, or gradual blood loss, especially from the stomach or colon…. We recommend you discuss your results with your family physician.”
Donors were later surveyed electronically about the action they took in the months after receiving the information letter. Approximately 25 per cent of the initial study population had repeat ferritin testing done when they returned to donate.
By the end of the study, the ferritin levels of about 12,000 donors were studied and the team concluded that iron deficiency is common among donors, with 23 per cent of female donors and 12 per cent of male donors having absent iron stores. Female sex, frequency of donation (number of donations in the year prior to ferritin testing), and for male donors, a borderline hemoglobin level near the cutoff, were risk factors for iron deficiency. And, 36 per cent of younger female first-time donors (below age 45) had low or absent iron stores prior to their first donation.
They also found that there may be a benefit to raising the acceptable hemoglobin range for males as other blood operators around the world have done (i.e. FDA, Council of Europe, ARC, UK). Males with borderline pass hemoglobin were more likely to have low iron stores, be very frequent donors, and fail their hemoglobin test at their next donation, suggesting that they are below their normal hemoglobin level and are at risk for developing iron deficiency anemia. And, they found that high-frequency donors are at greater risk.
“On repeat ferritin testing approximately one year later, study donors who initially had low ferritin levels had improved somewhat,” says Dr. Goldman. “Many donors with initially normal levels had decreased ferritin levels on retesting.”
These results indicate that all donors would benefit from more knowledge about iron needs. Donors who donate regularly might require iron supplementation to help maintain their iron levels.
The results of this large study have been published in the journal Transfusion.
Armed with knowledge, will donors protect themselves?
A follow up to the Ottawa-based study was recently “published in the journal Transfusion: Impact of informing donors of low ferritin results”. Here, the team found that after receiving a letter about low ferritin, donors returned to donate less frequently than they did before receiving the letter. In both the electronic survey and the qualitative phone interviews done with some of them, their understanding of their iron needs, and their compliance with iron therapy, was still not great.
These results also indicate that all donors would benefit from more knowledge about iron needs.
Changes to donor eligibility criteria
In addition to efforts to increase iron awareness among donors and as a result of the research team’s extensive studies of iron status of donors, two new measures have been introduced:
- The minimum acceptable hemoglobin levels for male whole blood donors will be increased to 130 g/L, effective Mar. 5, 2017.
- Female whole blood donors will only be allowed to donate every 84 days instead of 56, effective Dec. 10, 2016.
We are exploring ways in which we could test ferritin on selective donations, but this will not include testing at the clinic as the technology is not currently available. Additional studies are required to determine the optimal strategy and feasibility for donor ferritin testing. Canadian Blood Services will continue to qualify donors with a hemoglobin level at the clinic. As always, donors are encouraged to discuss their blood donor status with their physicians.
Positive results for one donor who received the "low ferritin" letter
The Canadian Blood Services’ National Contact Centre handles donor questions, queries and concerns. They recently heard a good news story from a 49-year-old male donor enrolled in Dr. Goldman’s national ferritin study. The donor at the heart of the story received a letter informing him that his ferritin level was low. He followed up with his doctor…
“This letter saved my life,” he wrote in a thank you email.
Turns out that he’d brought the letter to his doctor who ordered tests that revealed colon cancer. Three weeks following surgery he was 100 per cent cancer free. Had he not received and acted upon the letter his low-grade cancer could have been ended up being significantly more serious.
“In addition to helping others with my blood donations, Canadian Blood Services helped me!!” he wrote. “My family and I are very grateful.”
A positive result indeed!
“This response illustrates why we don’t want to simply assume that iron deficiency is due only to frequent donation, especially in male donors,” says Dr. Goldman. “It shows the health benefit of measuring ferritin levels and the importance of educating donors about iron.”
Further reading
- Iron facts page on blood.ca
- Research Unit: Protecting our lifeblood
- Iron deficiency in Canadian blood donors (Transfusion)
- Donor iron policy: from research to practice
- Impact of informing donors of low ferritin results
Canadian Blood Services – Driving world-class innovation
Through discovery, development and applied research, Canadian Blood Services drives world-class innovation in blood transfusion, cellular therapy and transplantation—bringing clarity and insight to an increasingly complex healthcare future. Our dedicated research team and extended network of partners engage in exploratory and applied research to create new knowledge, inform and enhance best practices, contribute to the development of new services and technologies, and build capacity through training and collaboration.
The opinions reflected in this post are those of the author and do not necessarily reflect the opinions of Canadian Blood Services nor do they reflect the views of Health Canada or any other funding agency.
Related blog posts
Researchers show that some methods used in the manufacturing of red blood cell units may be less damaging to the cells, which could reduce adverse reactions in transfusion recipients. This work may impact the future of how blood is collected in North America and around the world.
While blood transfusion is safer now than ever before, scientists continue to look for ways to reduce risk and ensure the healthiest possible outcomes for patients. A unique collaboration between Canadian Blood Services, The Ottawa Hospital and Université Laval has led to some interesting and...

